Katie's Procedure

Katie’s procedure – Limbal stem cell transplantation. Huge potential from this ground-breaking research.
This information is provided for informational purposes only. The stem cell transplant program is an investigative program, between the Queen Victorai Hospital and Centre for Sight. Centre for Sight is an independent organisation that offer exemplary private eye care and provides limbal stem cell transplants.
Reconstruction of the eye surface
The cornea, the area over the coloured part of the eye, is normally covered with a thin layer of “epithelial” cells similar to skin cells and as in the skin, the outer layer of cells are constantly shed and replaced from its surface. Damage to the limbus, the junction where the cornea (clear window) meets the sclera (white) from injuries or disease, the ability of the eyes to produce replacement corneal epithelial cells may be impaired. The cornea becomes cloudy, the vision deteriorates and the patient experiences considerable discomfort. A standard corneal graft will only temporarily replace the surface cells, as there will be no new cells to replace the old cells once they are shed. The corneal transplant will eventually fail.
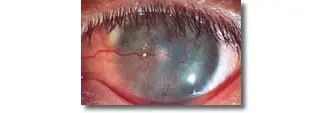
Preoperative status of patient’s eye showing vascularization and conjunctival invasion of the cornea surface.
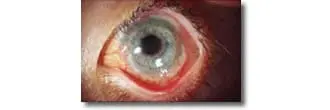
11 months post-op the sight has been restored to a visual acuity similar to pre-condition sight.
History and Background
Sheraz Daya previously Director of the Corneoplastic Unit and Eye Bank at the Queen Victoria Hospital initiated the stem cell research program through the Blond McIndoe Research Centre. Dr. Liz James developed the techniques for growing and expanding stem cell cultures and this work was later taken over by Dr. Nigel Jordan at the Queen Victoria Hospital
The source of cells is a small biopsy the size of a pin-head from the patients other eye, providing this is healthy and not damaged. In other cases, the stem cell donor tissue may come from a close relative or from eyes donated to the Queen Victoria Hospital Eye Bank. In all cases, presumed stem cells from the small tissue sample are grown in culture and then grafted onto the eye of the patient.
Over 60 procedures have now been performed between the Queen Victoria Hospital and Centre for Sight. The first patients were grafted in 1999, Outcome data is periodically reviewed and more than 70% were found to have a significant improvement in their condition with visual improvement. Two risk factors were identified that correlated with poor outcomes and these were 1) Active conjunctival inflammation and 2) Lid abnormalities. Great effort is taken to ensure these are both well controlled before embarking on stem cell transplantation.
One biological question we have tried to answer is whether the cultured donor cells have survived sufficiently long to be able to stimulate the regeneration of the patient’s own tissue. Using forensic DNA fingerprinting techniques, Justin Sharpe at Blond McIndoe Research has been able to show that donor cells can be demonstrated on the cornea over the first 3 to 4 months, and in spite of loss of donor cells, the ocular surfaces have been restored and have remained so long term. The donor stem cells have had a beneficial effect on the eye and seem to have attracted the patient’s own stem cells to take over. This we believe is a breakthrough and has considerable future implications. At a minimum, the need for long term immunosuppression following surgery may not be necessary. Additionally extrapolating on this work, there is the potential to regenerate other forms of tissue from the body’s own stem cells.
Surgeons
Mr. Sheraz Daya is Chairman and Medical Director of Centre for Sight and has resigned from the Queen Victoria Hospital. Patients who wish to undergo this type of surgery and avail of Mr. Daya’s considerable expertise and experience will have to be seen and treated on a private basis.
This work on stem cell transplantation to reconstruct the ocular surface has been presented nationally and internationally at the American Academy of Ophthalmology meeting (2003) and published in peer reviewed literature (Ophthalmology 2005 Mar;112(3):470-7 Outcomes surface reconstruction and DNA analysis of ex vivo expanded stem cell allograft for ocular surface reconstruction).