Laser cataract surgery on the NHS?

Should advanced femtosecond laser cataract surgery be available on the NHS? A view from Centre for Sight
Cataract surgery: powering up the femtosecond laser
18 July 2013 Chris Lo, featured on HospitalManagement.net
Femtosecond lasers are promising a dramatic improvement in cataract removal and other eye surgeries. What are the benefits of this technology for patients and care providers, and is it financially out of reach for public healthcare systems like the NHS?
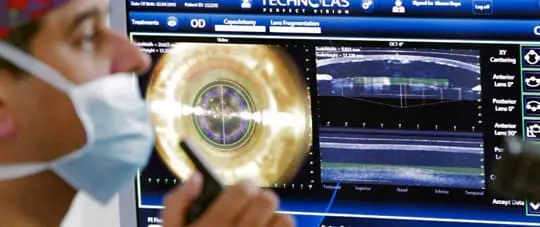
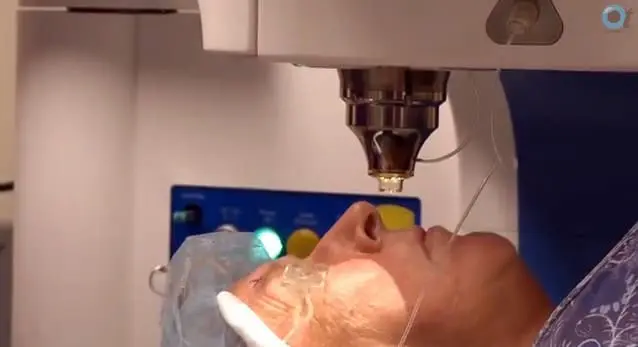
Baush and Lomb Victus Femtosecond Laser
The system software allows surgeons to create the perfect alignment for incisions.
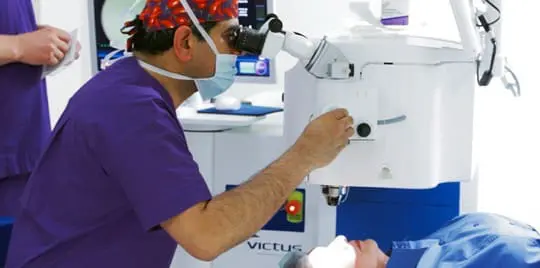
At the beginning of May, we visited Centre for Sight in East Grinstead, Sussex, for the UK’s first live 3D demonstration of Bausch + Lomb’s Victus femtosecond laser platform for cataract surgery. The packed audience of National Health Service (NHS) business managers and consultant ophthalmologists was kitted out with 3D glasses to provide a truer view as Dr. Sheraz Daya, leading eye surgeon and Centre for Sight’s medical director, worked through four cataract procedures over the course of 70 minutes.
“It only takes about six and a half to seven minutes to do the procedure”
Despite the straitened times facing the NHS and public health services all over the world, 2013 does seem like the right time to start showcasing femtosecond laser technology to potential buyers. The market for these advanced laser platforms, which use optic pulses lasting as little as one quadrillionth of a second to make extremely precise incisions for capsulotomy and lens fragmentation, has been maturing rapidly over the last few years from a development standpoint, but for now, the technology remains a relative rarity.
Dr. Daya, with whom we caught up a few weeks after the demonstration, confirms that femtosecond laser surgery is just starting to gain a foothold in the UK.
Cataract Symptoms
“I know of six other locations where they’re installed,” he says, pointing out that Centre for Sight was the first facility to use femtosecond lasers in the UK in 2004. “There are four different manufacturers out there, and they’re all competing for market share. This is a £400,000 ticket item; it’s not easy to find that kind of money in austere times, and most people are concerned about return on investment.”
As more femtosecond lasers are installed and used, evidence of the systems’ therapeutic benefits is beginning to accumulate. The platforms, which were originally indicated for use in LASIK laser eye surgery and have since expanded to cataract, refractive and therapeutic procedures, are being touted by their manufacturers and many of the surgeons who use them as an important advancement over existing manual methods.
“It only takes about six and a half to seven minutes to do the procedures.”
“The patient benefit is reproducibility on a scale that isn’t possible with human intervention”
One of the keys to the appeal of femtosecond lasers is the precision with which the platforms’ computer-guided lasers are able to make incisions, while the split-second duration of the pulses helps protect the surrounding tissue. “We actually reduce time inside the eye by doing the laser bits, and that can only be good for the eye,” says Daya. “So the advantages are precision, reproducibility and the duration inside the eye is reduced, which in turn reduces inflammation and the risk of infection.”
The reproducibility of outcomes is another important advantage, as Bausch + Lomb’s UK business director Craig Graham explains at the live demonstration. “The best surgeons are very skilled, but there is a distribution curve of surgeons, and even within the same surgeon there is a curve of how manually dexterous they are at a given operation, between operations. Victus automates that and brings in computer-guided lasers. So the benefit for the patient is reproducibility on a scale that just isn’t possible with human intervention. You still need a surgeon; you still need the clinical judgement around that, but it just gives the surgeon an extra tool to improve outcomes.”
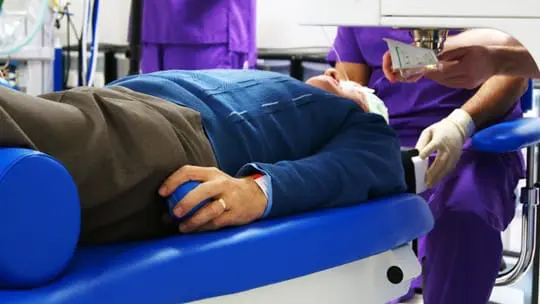
Hospitals and Clinics could Potentially Maximise Their ROI
As for healthcare providers, Graham notes that hospitals and clinics could potentially maximise their return on that hefty initial investment by attending to a higher volume of patients – the femtosecond cataract surgery takes around seven minutes to complete – and minimising the cost of post-operative complications.
“There are two trains of thought that could support [financial benefits],” Graham says. “One is a patient flow model, and that’s one of the things we’re looking at with centres like Centre for Sight – how do you optimise the asset base within a centre to provide higher volume throughput of surgeries, and [make them] more reproducible?
“This is a £400,000 ticket item; it‘s not easy to find that kind of money in austere times”
“The second aspect of that is if it’s more reproducible, the potential is for fewer complications, because complications add often-unseen cost into the procedures and into the healthcare system. So by approaching it both from the volume perspective but also the potential reduced complication rate, that’s where we see that the technology acquisition costs can be offset by service delivery costs down the line.”
As impressive as femtosecond lasers are, and as great as the potential benefits might be, Daya recognises that the technology is still in its infancy and will benefit from further development in a number of areas.
“The patient benefit is reproducibility on a scale that isn’t possible with human intervention.”
On the most fundamental level, formal clinical trials are required to conclusively prove the benefits that surgeons have been noticing in their daily work and to enhance the business case for wider adoption of femtosecond laser platforms.
“The benefits are hypothetical,” he says. “They make sense and they’re intuitive, but ultimately you need a randomised, controlled study to determine the benefit of this. People are already starting to work on it in different places; I know in Singapore, they’ve got [a trial] going at the moment.”
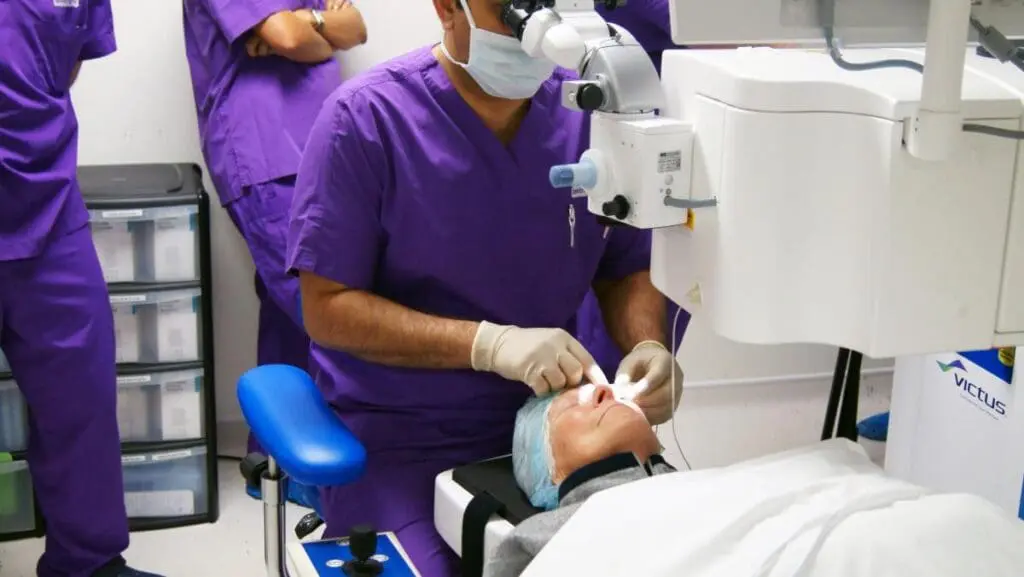
Daya also notes that the improvement of patient flow through faster, computer-guided surgeries – central to making femtosecond lasers viable in public as well as private healthcare – could be pushed further as the arrangement and use of the device is tweaked. The current status quo for femtosecond lasers is to have a surgeon supervising the laser work, then moving the patient to a separate station in the operating theatre to carry out the lens removal.
Graham says there is interest from public healthcare, as proved by the many NHS consultants at the demonstration, but acknowledges the dilemma. “It’s an interesting question, because the reinvestment rates for cataracts are static, and we all know the economic pressures faced by the UK economy.”
Daya draws a similar line between surgeons wanting the best for their patients and the structural drawbacks of the NHS. “They’re incredibly interested, and I think they’d like to do the same sort of modelling of how they could make it fly. But you know what the NHS trusts are like; it depends which trust you’re in, and what the management is like. The place can fall apart and change overnight, depending on who the chief executive is.”
Author Information
Authored by Sheraz Daya MD FACP FACS FRCS(Ed) FRCOphth, Consultant Ophthalmic Surgeon & Medical Director, June 2019.
Next review due August 2025