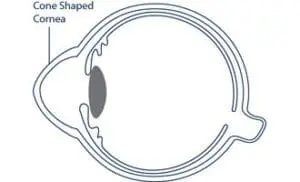
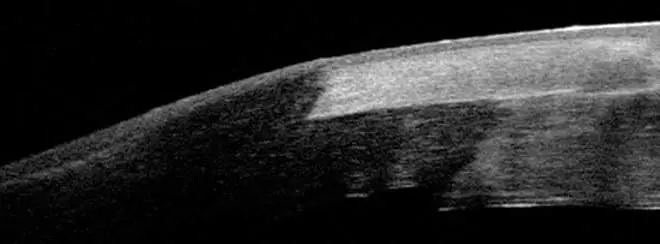
Surgeons at Centre for Sight are internationally renowned for their expertise in Keratoconus and Corneal problems. Centre for Sight’s medical director is on numerous boards and committees related to Keratoconus and is on the founding editorial board of the peer-reviewed publication Keratoconus, as well as a founding member of the Keratoconus Expert Group, an international group of Keratoconus specialists. He was involved as a panellist in the Global Consensus Working Group the findings and conclusion of which were recently published in the journal Cornea.
Click here to read more about keratoconus aftercare treatment.